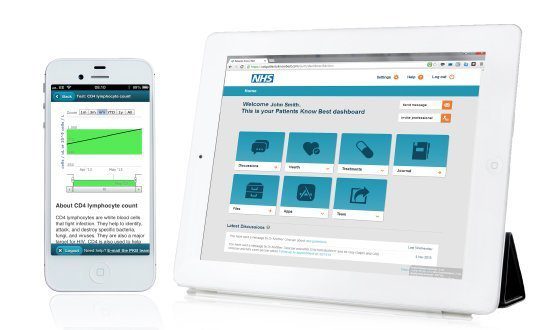
The Northern Queensland Primary Health Network is deploying a shared care platform to GPs in North Queensland. The care planning platform, INCA, developed by the health IT company Precedence Health Care, enables health professionals to manage patient health data, create and monitor care plans, and share information digitally.
This system allows the creation of Medicare-compliant GP management plans and team care arrangements, which can be automatically shared with the care team. It also enables GPs to allocate tasks and send automatic reminders for actions needing completion, track and monitor adherence to a plan, and store all approved and shared documentation in one record.
Moreover, INCA…
Continue Reading